Customer Updates: Stryker Network Disruption > Read Now
Our customers
Committed to your success
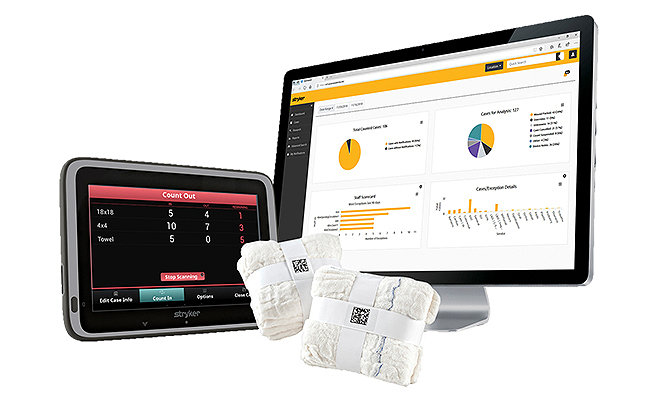
From teaching institutions to community hospitals, to government VAs and surgery centers, more organizations are choosing the SurgiCount System. There are more than 500 facilities using the SurgiCount System, including 60% of U.S. News & World Report’s top 10 Honor Roll Hospitals.15
Straight from the source
It’s true. We have 100% belief in our SurgiCount System and here’s the story direct from our customers.
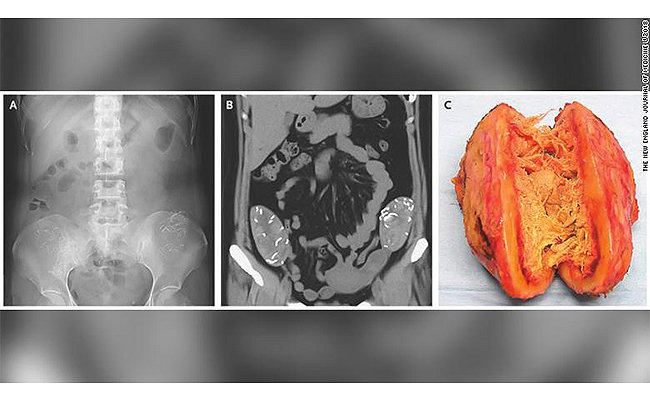
Retained surgical sponges occur in roughly a dozen patients a day in the U.S.17
9100-003-604 Rev None
Stryker Corporation or its divisions or other corporate affiliated entities own, use or have applied for the following trademarks or service marks: SAFE-T Lap, Safety-Sponge, Stryker, SurgiCount, SurgiCount360, and SurgiCounter. All other trademarks are trademarks of their respective owners or holders.
9100-003-611 Rev None