Customer Updates: Stryker Network Disruption > Read Now
13-Oct-2020
At Stryker, we care about every patient's journey. And through innovative technologies, we empower surgeons to help improve that journey.
Every year in the United States, about 250,000 cases of breast cancer are diagnosed in women and about 2,300 in men. And of those numbers, about 42,000 women and 510 men in the U.S. die each year from breast cancer.1
In the last 35 years, since Breast Cancer Awareness Month was created, our world has made considerable progress in the evolution of treatment and recovery—not just physical, but emotional too. Stryker has proudly been part of that progress. As we work closely with our customers, we listen and build understanding, and then innovate based on what we learn, empowering healthcare providers to deliver better outcomes.
Improving visualization for breast reconstruction
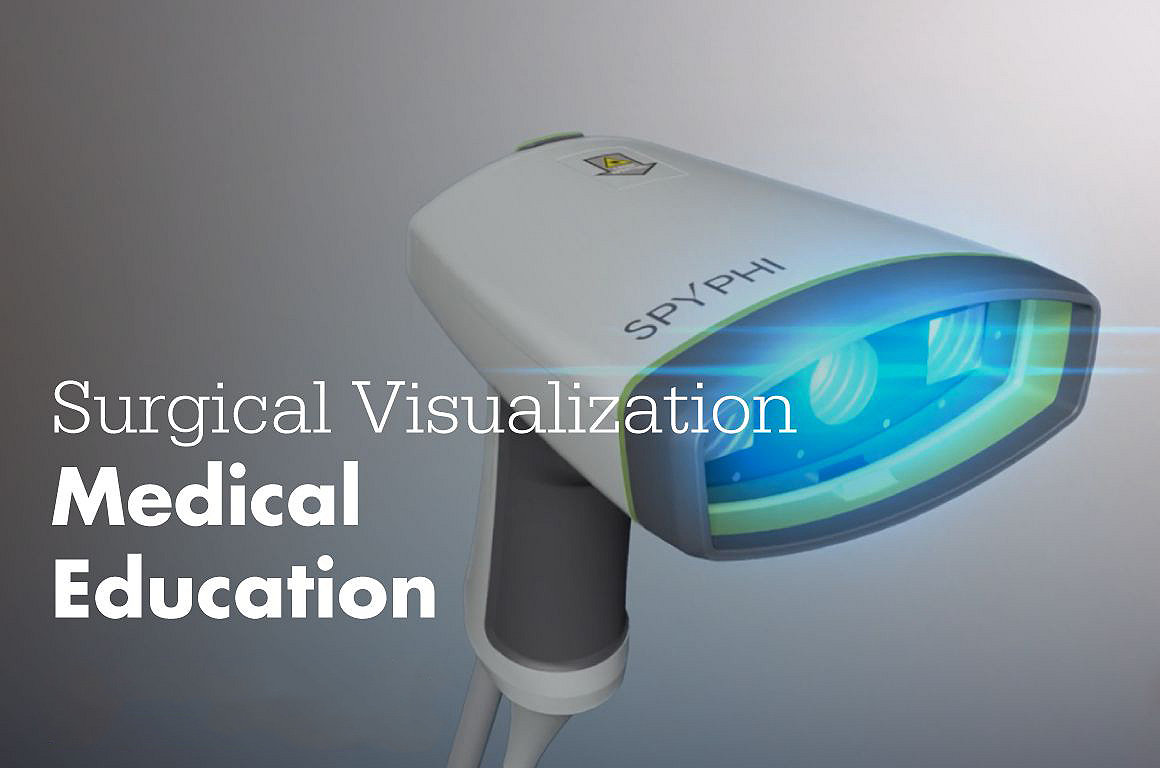
Adequate blood flow is crucial to surgical success and the body’s ability to heal. Even a few hours of impaired blood flow can cause damage that can lead to post-operative complications. Advancements in technology, such as our SPY Fluorescence Imaging, can help provide surgeons with real-time visualization of tissue perfusion during breast reconstruction, which may help a surgeon make certain decisions to improve surgical outcomes.2 SPY-PHI Fluorescence Imaging technology works by using a near-infrared low powered laser light source to stimulate a fluorescent imaging agent that has been injected into a patient's bloodstream. This makes it possible for surgeons to visualize blood flow in real-time.
Meet Barbara, who made the decision to get a bilateral mastectomy and bilateral breast reconstruction when she learned she had an aggressive form of breast cancer. Her surgeon, Dr. Charles Kays, from Wilmington Plastic Surgery, in Wilmington, North Carolina, took advantage of Stryker’s innovative SPY Fluorescence imaging technology during the complicated operation. The reconstructive operation was a success, and Barbara was up and around in just a few days and fully back in action after only four weeks.
Minimizing scarring for a psychological and emotional recovery
While some may see their scars as an empowering symbol, many do not. In fact, 87%
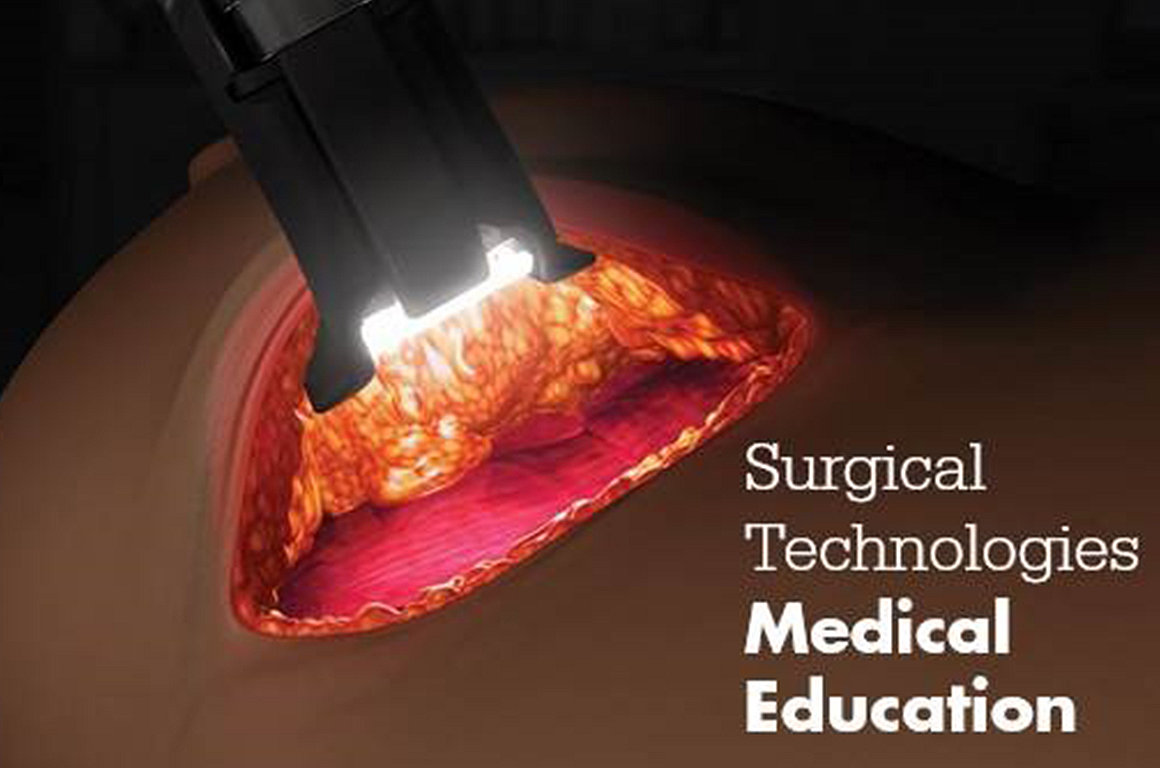
of women are self-conscious due to scars from breast cancer surgery.3 There are a number of surgical options available, including oncoplastic surgery techniques, an advanced surgical approach in which breast surgeons remove cancerous tissue through a single incision made in inconspicuous areas to minimize visible scarring. Surgeons can use oncoplastic techniques in either a mastectomy or lumpectomy procedure. Through thermally-cool, volumetric illumination, our Illuminated Instruments provide surgeons with enhanced visualization that offer positive physical and psychosocial wellbeing for patients by providing oncologic outcomes equal to traditional techniques.4
Meet Dr. Anne Peled, an oncoplastic surgeon. On the day she was getting ready to perform a double mastectomy and breast reconstruction, her phone rang and she learned that the disease she spent her life treating had found her. “I had to remind myself what I tell my patients,” she said. “That this is very treatable and, in many cases, curable.”
Dr. Peled was able to put together an amazing team of caring and talented clinicians. She got through treatment smoothly and relatively easily, thanks, in part, to the type of hidden scar surgery she performs on her own patients. And today, she speaks with every patient with a unique level of shared understanding.
Supporting surgeons, so they can support patients
These offerings are designed to help advance product and procedural knowledge and skills, improve customer competence and confidence, and lead to better patient outcomes.
Further your understanding
Resources for patients
1. Basic Information About Breast Cancer. CDC.gov. https://www.cdc.gov/cancer/breast/basic_info/index.htm#:~:text=Each%20year%20in%20the%20United,breast%20cancer%20than%20White%20women. Accessed October 5, 2020.
2. Newman M, Samson M, Tamburrino J, Swartz K, “Intraoperative Laser-Assisted Indocyanine Green Angiography for the Evaluation of Mastectomy Flaps in Immediate Breast Reconstruction” Plastic Surgery | Journal of Reconstructive Microsurgery. 2010 Sep;26(7):487-92. doi: 10.1055/s-0030-1261701. Epub 2010 Jun 10.
3. LIT 12728 Rev A Wakefield Research Data Report: Survey of Breast Cancer Surgery Patients
4. Chand, N. et al. “Patient Reported Outcomes Are Better After Oncoplastic Breast Conservation Than After Mastectomy and Autologous Reconstruction.” International Open Access Journal of the American Society of Plastic Surgeons. (2017)
SYK CORP 2020-10-41. ECO101133