Customer Updates: Stryker Network Disruption > Read Now
28-Sep-2023
The Sage PrimaFit External Urine Management for the Female Anatomy helped decrease CAUTI rates 72%7
Clinical Nurse Specialists initiate a quality improvement program to reduce CAUTI prevalence and harm
Catheter-associated urinary tract infections (CAUTIs) are one of the most common healthcare-acquired infections (HAIs)-making up nearly 40% of all HAIs.1 Of these:
- Approximately 75% are associated with urinary catheters2
- Up to 95% of urinary tract infections (UTIs) in the intensive care unit (ICU) are associated with catheters3
- Up to 25% of hospital patients have a urinary catheter at some point during their stay2
CAUTIs are associated with increases in morbidity, mortality, and costs.
- Estimated 449,334 CAUTI harm events per year4
- Estimated 13,000 annual UTI related deaths5
- The cost of a CAUTI is approximately $600 with up to $340 million spent in healthcare per year4
Background
Terrie Beeson and Carmen Davis are Clinical Nurse Specialists at University Hospital, a part of Indiana University Health System. In an effort to reduce CAUTI prevalence and harm, Beeson and Davis evaluated strategies designed to help decrease indwelling urinary catheter usage in female patients. Additionally, they conducted data collection surveys exploring workflow impact on nursing practice with the use of a urine management system in acute and critically ill women.
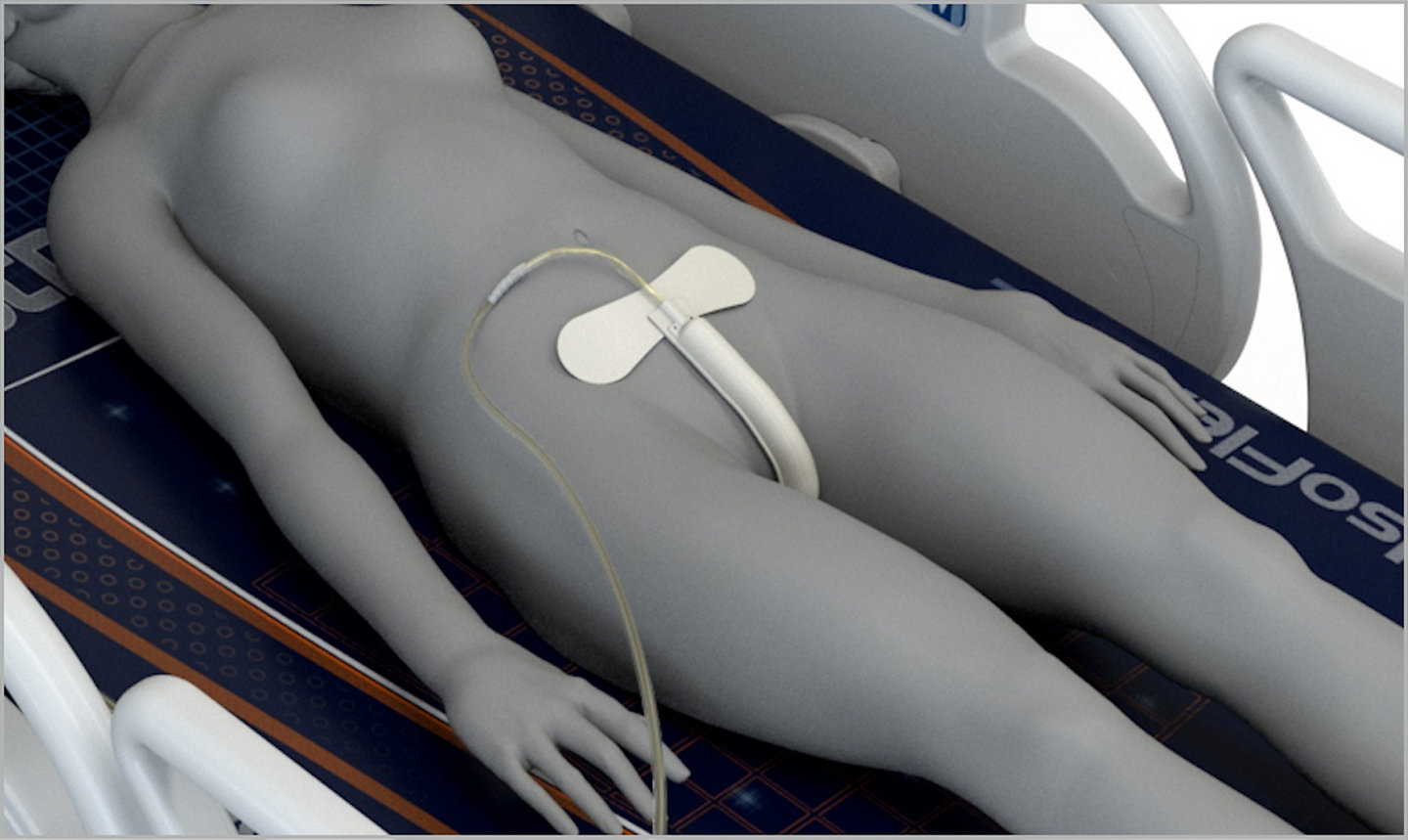
Intervention
Beeson and Davis initiated a quality improvement pilot program using an external female urine management system in an 18-bed adult SICU. Female patients were identified for early removal of indwelling urinary catheters during interdisciplinary rounds for CAUTI prevention. Daily rounds included a review of the Centers for Disease Control (CDC) indications for ongoing catheter need. For female patients who remained incontinent after a catheter was removed or when output management was needed, the external female urine collection device was applied. The device was used on a range of surgical and medical patients with variable ages and body mass indexes.6
CAUTI rates and Standard Infection Ratio (SIR) metrics were compared. For data collection, the preimplementation time was April to September 2016 and the post-implementation was April to September 2017.6
Results
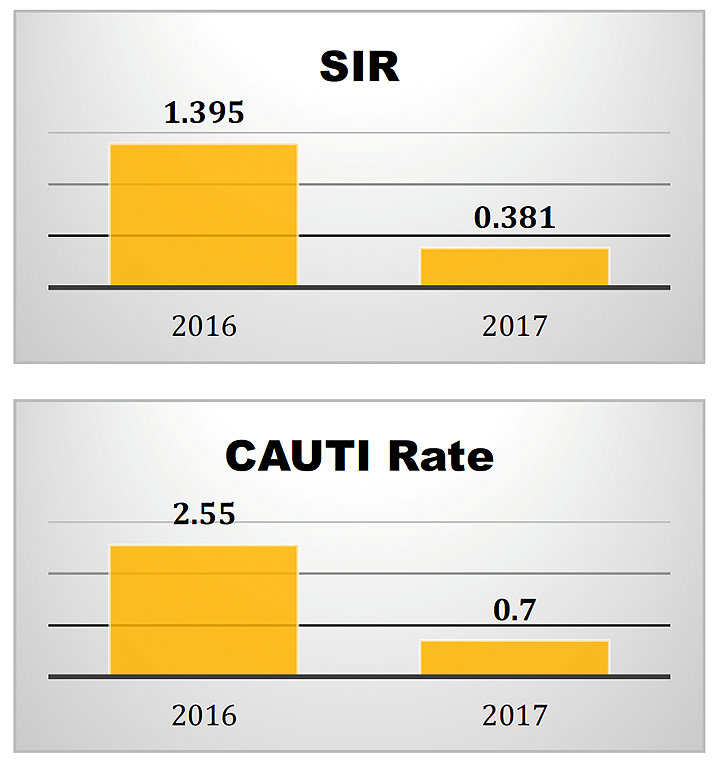
- SIR decreased considerably in the six-month pilot time of 2017, from 1.395 to 0.381.6
- CAUTI rates during the pilot decreased 27%, from 2.55 in 2016 to 0.70 in 2017.6
In addition, nurses caring for these patients reported satisfaction associated with a decreased workload of frequent linen changes, the ability to capture and record drainage output, and general excitement about a viable alternative to help keep patients safe from infection and skin injury. Nurses surveyed agreed that the product helped to manage female urinary incontinence.7 Patients also verbalized satisfaction with the use of the female external urine collection device.8
Conclusion
The Sage PrimaFit External Urine Management System for Females can be a viable alternative to an indwelling urinary catheter or intervention for urinary incontinence. The female external urine collection device can minimize the risk of infection for female patients.8
Learn more
To learn more about PrimaFit how can help manage urinary incontinence for your patients with female anatomy and promote early catheter removal, click here.
About the Clinicians
With nearly 40 years of experience, Terrie Beeson MSN, RN, CCRN, ACNS-BC, and 20 years of experience, Carmen R. Davis MSN, RN, CCRN, CNS-BC are practicing critical care clinical nurse specialists in an academic tertiary referral center (Surgical and Medical Intensive Care Units, respectively). They are responsible for providing clinical leadership and promoting optimal patient outcomes. In addition, they collaborate with all members of the healthcare team to design, implement, and provide safe, cost-effective, evidence-based care strategies.
*Both clinicians are consultants for Sage/Stryker.
1. Saint S, et al., Preventing Hospital-Acquired Urinary Tract Infection in the United States: A National Study, Clinical Infectious Diseases (CID), 2008;46:243-50.
2. Centers for Disease Control and Prevention. Healthcare-associated Infections: Catheter-associated Urinary Tract Infections (CAUTI). Available at file:///Volumes/company/_PMRs/White%20Papers/PrimaFit%20Customer%20Highlight/Catheterassociated%20Urinary%20Tract%20Infections%20(CAUTI)%20_%20HAI%20_%20CDC.html Accessed October 15, 2018.
3. Chenoweth CE, Gould CV, Saint S, Diagnosis, Management, and Prevention of Catheter-Associated Urinary Tract Infections, Infectous Disease Clinics of North America, 2014 March;28(1):105-19.
4. Scott RD, The direct medical costs of healthcare-associated infections in US hospitals and the benefits of prevention. Division of Healthcare Quality Promotion National Center for Preparedness, Detection, and Control of Infectious Diseases Coordinating Center for Infectious Diseases Centers for Disease Control and Prevention, March 2009.
5. Klevens RM, et al., Estimating Health Care-Associated Infections and Deaths in US Hospitals, 2002. Public Health Reports, March-April 2007;122(2):160-66.
6. Beeson T, Davis C, Vollman K, Chasing Zero Catheter Associated Urinary Tract Infections (CAUTIs) through Implementing a Novel Female External Urine Collection Device in a Tertiary Academic Surgical Intensive Care Unit (SICU) Presented at APIC 2018.
7. Beeson T, Davis C, An Innovative Technique for Managing Female Urinary Incontinence in Acute and Critically Ill Women. Presented at Wound Ostomy and Continence Nurses annual conference. June 3-6, 2018 Philadelphia, PA. 8. Beeson T, Davis C, Urinary Management with an External Female Collection Device. Journal of Wound, Ostomy, and Continence Nursing, 2018;45(2):187-89.
802794
