Customer Updates: Stryker Network Disruption > Read Now
Strategies to help address risk factors that may lead to pneumonia in acute care hospitals
29-Aug-2023
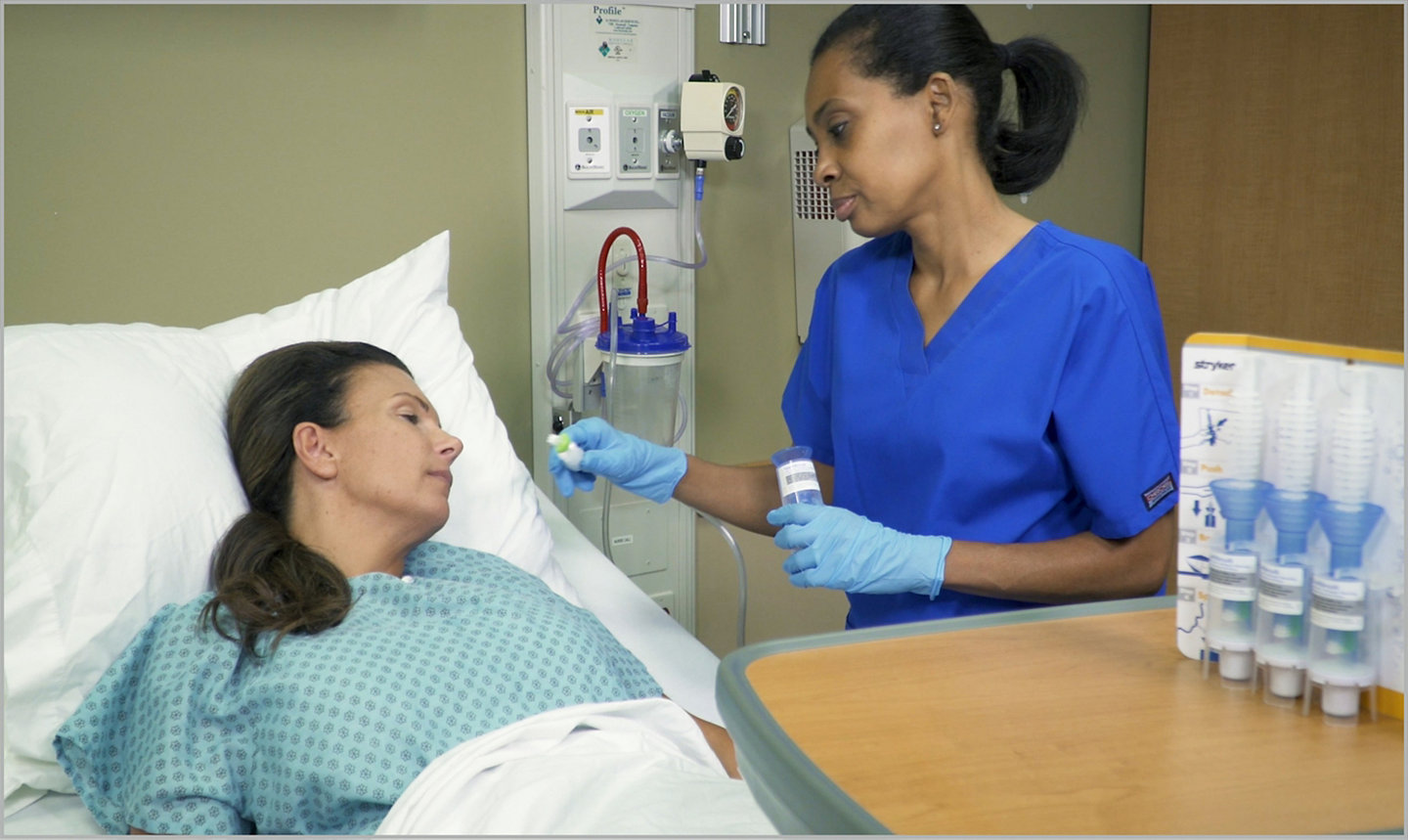
SHEA/IDSA/APIC Practice recommendation update adds basic practice of daily toothbrushing
This expert guidance document was created to help acute hospitals prioritize and implement strategies to address risk factors that may lead to ventilator-associated pneumonia (VAP), ventilator-associated events (VAE), and non-ventilator hospital-acquired pneumonia (NV-HAP). This 2022 update was based on initial recommendations published in 2014 and sponsored by the Society for Healthcare Epidemiology (SHEA). It is the product of a collaborative effort led by SHEA, the Infectious Diseases Society of America, the American Hospital Association (ICHE), the Association for Professionals in Infection Control an Epidemiology (APIC), and The Joint Commission, with major contributions from representatives of a number of organizations and societies with content expertise. This is a summary of this team’s recommendations for strategies to decrease NV-HAP.
Interventions that may lower NV-HAP rates with little risk of harm are:
- Provide regular oral care. This is the most commonly studied strategy to address risk factors that may lead to NV-HAP and a possible benefit has been shown. Recommendation is to brush teeth daily given its benefits of oral health and possible positive impact.
- Early diagnosis and treatment of dysphagia, especially among neurologically impaired post-stroke patients.
- Mobilize patients early, taking into account the risk of falls.
- Take steps to reduce transmission of viral infections such as symptom screening of patients and employees, surveillance testing of all admitted patients, universal masking when respiratory virus rates are high.
- Implement best practice prevention bundles of care that have been shown to address risk factors that may lead to NV-HAP and include all interventions included in bundle. The contribution and effectiveness of each bundle element remains unknown however data supports bundle implementation to decrease risk of NV-HAP.
Interventions with very little data that show impact on NV-HAP are:
- Elevating the head of bed is recommended to address risk factors that may lead to VAP, however there is very little evidence associated with NV-HAP reduction.
- Stress ulcer prophylaxis may reduce risk for NV-HAP, however there are no randomized trials assessing the impact of acid reducing medications on NV-HAP.
This update is important as hospitals strive to improve safety and care for their patients. These strategies have been provided by a national, multidisciplinary team of experts to recommend best treatment practices and avoid outcomes associated with dangerous and costly hospital-acquired infections.
To read the full practice recommendation click here.
To learn more about products that can help address the risk factors for hospital-acquired pneumonia, click here.
Reference:
1. Klompas M, et al., Strategies to prevent ventilator-associated pneumonia, ventilator-associated events, and nonventilator hospital-acquired pneumonia in acute-care hospitals: 2022 Update, Infection Control & Hospital Epidemiology, 2022, 43: 687-713.
765900

